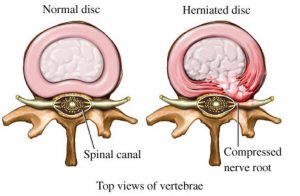
A disc herniation can be a debilitating experience. The sudden sharp pain in the back will tell you something isn’t right. They can affect all aspects of life – from sitting in the car to trying to sleep. Some disc injuries can also cause numbness, weakness, or altered sensation down the leg. We understand the draining effect this can have, so we laid out our tips on finding relief from a disc herniation.
Anatomy of Intervertebral Discs
The spine consists of 24 bony segments called vertebrae. Between each one of these vertebrae are spongy, gel-like structures called intervertebral discs. These discs act as shock absorbers in the spine, ensuring the bones don’t rub across each other. They also have the added benefit of creating joints in the spine, allowing it to move about with a broad, global motion. These discs have sturdy outer rings of tissues called the annulus fibrosis and a jelly-like center called the nucleus pulposus. A great visual for the intervertebral disc is to think of a jelly-filled donut.
As we age, these discs lose fluid and dry out. This fluid loss causes the center of the disc to bulge outward into the outer rings and may cause pain. We classify this as a bulging disc. As degeneration of the disc continues, or with the addition of significant stresses to the lower back, the inner gel may eventually rupture through the outer ring, causing a herniated disc. With our jelly donut example, think of squeezing on the donut until the gel tears through the walls and oozes out.
In some cases, the fragmented disc material can inflame or put pressure on the spinal nerves in the area. This nerve compression can create numbness, weakness, or altered sensation in one or both legs.
Risk Factors for a Disc Herniation
- Age and Gender – the highest incidence in men aged 25 to 45 years old
- Obesity – being overweight adds stress to the discs
- Sedentary life – lack of movement and weak core strength increase chances of disc herniation
- Smoking – smoking reduces the oxygen supply to discs and promotes quicker degeneration
- Improper lifting – using your back muscles to lift instead of your legs. Twisting while lifting
- Repetitive activities that strain your spine – jobs that require constant lifting, bending, twisting, or pulling
- Frequent driving – staying seated for extended periods can increase the pressure on your disc
Diagnosis of a Disc Herniation
 For any patient with a complaint of back pain, your doctor will first go through a thorough consultation and history of the problem. Many disc injuries present with a history of improper lifting and twisting. These patients will also have pain getting out of bed and with activities like coughing or sneezing.
For any patient with a complaint of back pain, your doctor will first go through a thorough consultation and history of the problem. Many disc injuries present with a history of improper lifting and twisting. These patients will also have pain getting out of bed and with activities like coughing or sneezing.
Next, the healthcare provider will move forward with a physical exam. They can check things from muscle strength to nerve function, as well as the region’s overall mobility. There are also several movement tests that, if positive, increase the suspicion of a disc injury.
Advanced imaging can aid your doctor’s diagnosis by viewing the spine’s bones, muscles, and soft tissue. Some examples of these imaging options include X-rays, CT, MRI, and discograms.
Treatment of a Disc Herniation
Conservative care should always be the first treatment for disc injuries. The exact treatment parameters will depend on your age, health, therapy tolerance, and overall clinical picture. Disc herniation treatment always begins with reducing the symptoms in the arms or legs. It is imperative to prevent further neurological loss by decompressing the pinched nerve (if present) and reducing the disc herniation.
Care includes chiropractic adjustments to mobilize the area and soft tissue therapies that the patient can tolerate. Home care consists of repetitive motions to a position of relief and spinal stabilization exercises. Ice and anti-inflammatories may also aid in the healing process.
While avoiding all physical activity while the segment is injured may be tempting, this is ill-advised. Lack of motion can lead to muscle weakness and overall joint stiffness. Instead, we recommend continual movement through stretching and other low-impact activities, like walking.
Body Positioning
Avoiding reaggravation is essential to a quicker recovery from a disc herniation. We outline a few everyday activities you perform every day and proper adaptations to reduce the chances of injury.
Going from Sit-to-Stand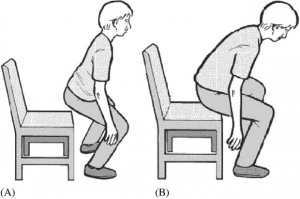
- Start in a seated position at the edge of the chair with both feet directly under your knees
- Initiate the movement by driving your legs into the ground
- Use your hips and knees and knees to propel you upward
- Avoid bending the lower back
- Keep the torso upright while rising from the chair.
Brushing your Teeth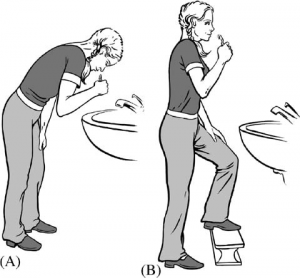
- Keep the chest and torso tall while brushing your teeth
- If you need to bend forward to rinse your mouth, squat down at the hips, avoiding flexion of the back
- Keep the chest tall while you lean forward
- You may also put a small stool under one foot to aid. Or you can open the cabinets below your sink and put a foot on the shelf. This allows more effortless motion of the hips without straining the back.
Picking up Objects from the Ground
- Bend from the knees and keep the chest lifted to lower yourself down to the object
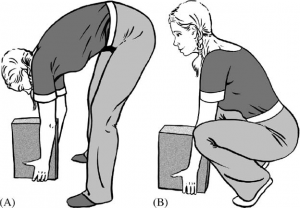 When lifting, keep the spine tall and upright by hinging from the hips and knees
When lifting, keep the spine tall and upright by hinging from the hips and knees- Have the object directly in front of you, limiting too much forward lean
- Be sure to focus on keeping your lower back’s natural curve
- Avoid lifting immediately after being in a seated position for a prolonged period
Preventing a Disc Herniation
Current research suggests that you may not be able to eliminate the chances of developing a disc herniation entirely.2 However, you can take steps to reduce your risk of injury.
- Always use safe lifting techniques – bend at your knees and not your waist
- Maintain a healthy weight
- Do not remain seated for long periods – get up and stretch
- Perform exercises regularly that strengthen the back, legs, and abdomen muscles.
Whether seeking relief from chronic pain or simply aiming for optimal health, your Livonia chiropractor guides you every step of the way. Contact our office to schedule an appointment by Clicking Here or giving us a call today: 734-427-6333